Sebaceous Carcinoma of the Eyelid
Definition: Sebaceous carcinoma is a malignant neoplasm arising in sebaceous glands that is characterized by extensive lipid production.
Incidence/Prevalence: Sebaceous carcinoma is considered the second most common malignant neoplasm of the eyelid accounting for about 5% of all primary eyelid malignancies (basal cell carcinoma 90%, squamous carcinoma 4% and malignant melanoma 1%). About 70% occur in women and the mean age range from a variety of series is between 57-72 years.
Etiology: Sebaceous carcinoma of the eyelids may arise in the meibomian glands of the tarsus, the glands of Zeis in the skin of the eyelid, or the sebaceous glands of the caruncle.
Clinical Findings: The key clinical feature is thickening of the eyelid which is present in about 57% of cases. About 43% present with a nodule. Clinical diagnosis is often missed (about 68% of the time) or delayed because of this lesion’s propensity to mimic or accompany a chalazion, and/or produce chronic blepharoconjunctivitis. There are more Meibomian glands in the upper lid than the lower lid. This may account for the greater frequency of sebaceous carcinoma in the upper lid. When sebaceous carcinoma is suspected clinically, the pathologist should be alerted so a strategy can be put in place for documentation of lipid within tumor cells, e.g. glutaraldehyde and paraformaldehyde fixation with osmication or frozen sections for lipid stains. Survival rates for sebaceous carcinoma are perhaps slightly worse than those for squamous cell carcinoma but have improved in recent years as a result of increased awareness, earlier detection, more accurate diagnosis, and appropriate treatment. Metastases first involve regional lymph nodes and occur in about 30% of cases.
Histopathology: Sebaceous carcinoma is initially misdiagnosed by the general pathologist about 50% of the time; the diagnosis is usually given as squamous carcinoma. This is not an egregious error because both sebaceous and squamous carcinoma require complete excision. There is some evidence that the prognosis is similar for both entities. Sebaceous carcinoma infiltrates and destroys the architecture of the eyelid. In the macroimage of the cross section of an eyelid one can identify the epidermis (arrow 1), normal cilia (arrow 2) and superficial dermal hemorrhage (arrow 3). Complete effacement of Meibomian glands of the eyelid is due to infiltration by a white tumor (number 4) that appears to have its center where the Meibomian glands usually are located in the lid. Even in the gross, glands of Zeis are visualized; note the cilia emanating from the lid (arrow 5).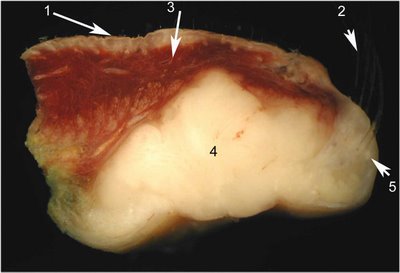
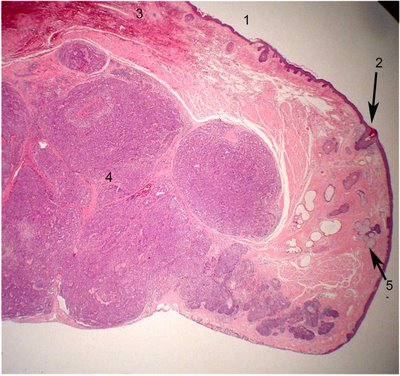 A comparison is afforded by this histologic section that is taken correlatively within about 100 microns from the gross photo. The structures are numbered similarly for your comparison. In the higher magnification image, the malignant neoplasm features large cells with vesicular bubbly cytoplasm (arrow 6). The clear foamy cytoplasm represent empty spaces presumably occupied by lipid prior to organic solvent extraction during processing.
A comparison is afforded by this histologic section that is taken correlatively within about 100 microns from the gross photo. The structures are numbered similarly for your comparison. In the higher magnification image, the malignant neoplasm features large cells with vesicular bubbly cytoplasm (arrow 6). The clear foamy cytoplasm represent empty spaces presumably occupied by lipid prior to organic solvent extraction during processing. 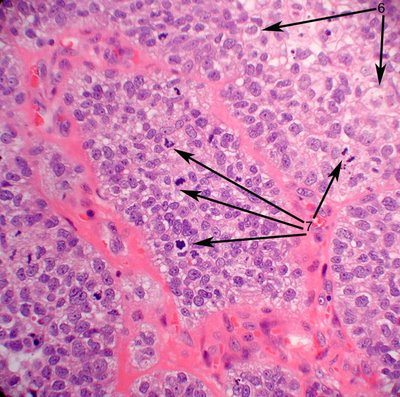 The nuclei are enlarged and have prominent nucleoli. Mitotic figures abound (arrow 7). The demonstration of lipid within the cytoplasm of tumor cells by special stains is a prerequisite for the diagnosis. Our laboratory prefers to osmicate the tissues with osmium tetroxide, which is a classic method of fixing lipid. This can be done on formalin fixed material which provide the pathologist flexibility in dealing with a wide range of clinical colleagues. One micron plastic sections are stained with toluidine blue. The lipid appears bright green in section (arrows 8).
The nuclei are enlarged and have prominent nucleoli. Mitotic figures abound (arrow 7). The demonstration of lipid within the cytoplasm of tumor cells by special stains is a prerequisite for the diagnosis. Our laboratory prefers to osmicate the tissues with osmium tetroxide, which is a classic method of fixing lipid. This can be done on formalin fixed material which provide the pathologist flexibility in dealing with a wide range of clinical colleagues. One micron plastic sections are stained with toluidine blue. The lipid appears bright green in section (arrows 8). 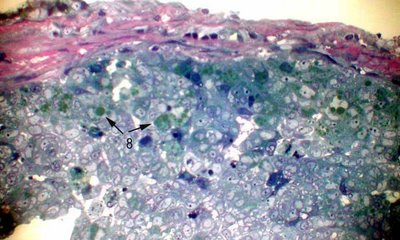 Alternatively oil red O or Sudan black staining, can be performed on frozen section, but typically these may be quite difficult to interpret. Adequate frozen sections are notoriously difficult to obtain from skin. Immunohistochemistry may be helpful when documentation of lipid is not feasible (paraffin sections are all that is available). Positive reactivity to antibodies to CAM5.2 and EMA are often positive in sebaceous carcinoma and negative in squamous carcinoma and basal cell carcinoma, respectively.
Alternatively oil red O or Sudan black staining, can be performed on frozen section, but typically these may be quite difficult to interpret. Adequate frozen sections are notoriously difficult to obtain from skin. Immunohistochemistry may be helpful when documentation of lipid is not feasible (paraffin sections are all that is available). Positive reactivity to antibodies to CAM5.2 and EMA are often positive in sebaceous carcinoma and negative in squamous carcinoma and basal cell carcinoma, respectively.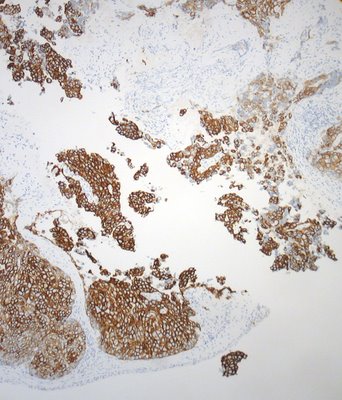 The illustration shows anti-CAM5.2 reacting strongly with infiltrative nests cells of a sebaceous carcinoma. Pagetoid spread of sebaceous carcinoma is quite typical with tumor cells replacing the epithelium. Clusters and single cells may infiltrate the epithelium at various levels. Another pattern in the conjunctiva is that of complete replacement of conjunctival epithelium by tumor cells. A rare variant of sebaceous carcinoma involves only the epidermis and conjunctiva without demonstrable invasive tumor. The distribution of sebaceous carcinoma often is irregular and may feature skip lesions. The prudent surgeon will often map the tumor with tiny multiple biopsies from numerous sites on both lids prior to or during the excision of the main tumor.
The illustration shows anti-CAM5.2 reacting strongly with infiltrative nests cells of a sebaceous carcinoma. Pagetoid spread of sebaceous carcinoma is quite typical with tumor cells replacing the epithelium. Clusters and single cells may infiltrate the epithelium at various levels. Another pattern in the conjunctiva is that of complete replacement of conjunctival epithelium by tumor cells. A rare variant of sebaceous carcinoma involves only the epidermis and conjunctiva without demonstrable invasive tumor. The distribution of sebaceous carcinoma often is irregular and may feature skip lesions. The prudent surgeon will often map the tumor with tiny multiple biopsies from numerous sites on both lids prior to or during the excision of the main tumor.
Treatment: In most cases complete removal of the malignant neoplasm is the treatment of choice. Exenteration is sometimes (about 13% in some series) performed for larger or deeply invasive tumors. Because sebaceous carcinoma tends to be multifocal, an approach using Moh's surgery may result in incomplete removal of the tumor.
Prognosis: The recurrence rate is about 18% in the hands of Shields et al. and 8% produce distant metastases. The mortality due to sebaceous carcinoma has been estimated by others to be about 3%.
References:
Muquit et al. Eye 2004 18:49-53.
Shields JA et al. Survey of Ophthalmology 2005; 50:103-122
